Barbados is mobilizing a comprehensive national response to its escalating non-communicable disease epidemic with the inaugural Live Stronger Longer wellness conference scheduled for May 18-19. Organized by the Diabetes and Hypertension Association of Barbados (DHAB) in partnership with Republic Bank Barbados Limited, the event marks a strategic pivot from public awareness to actionable health solutions.
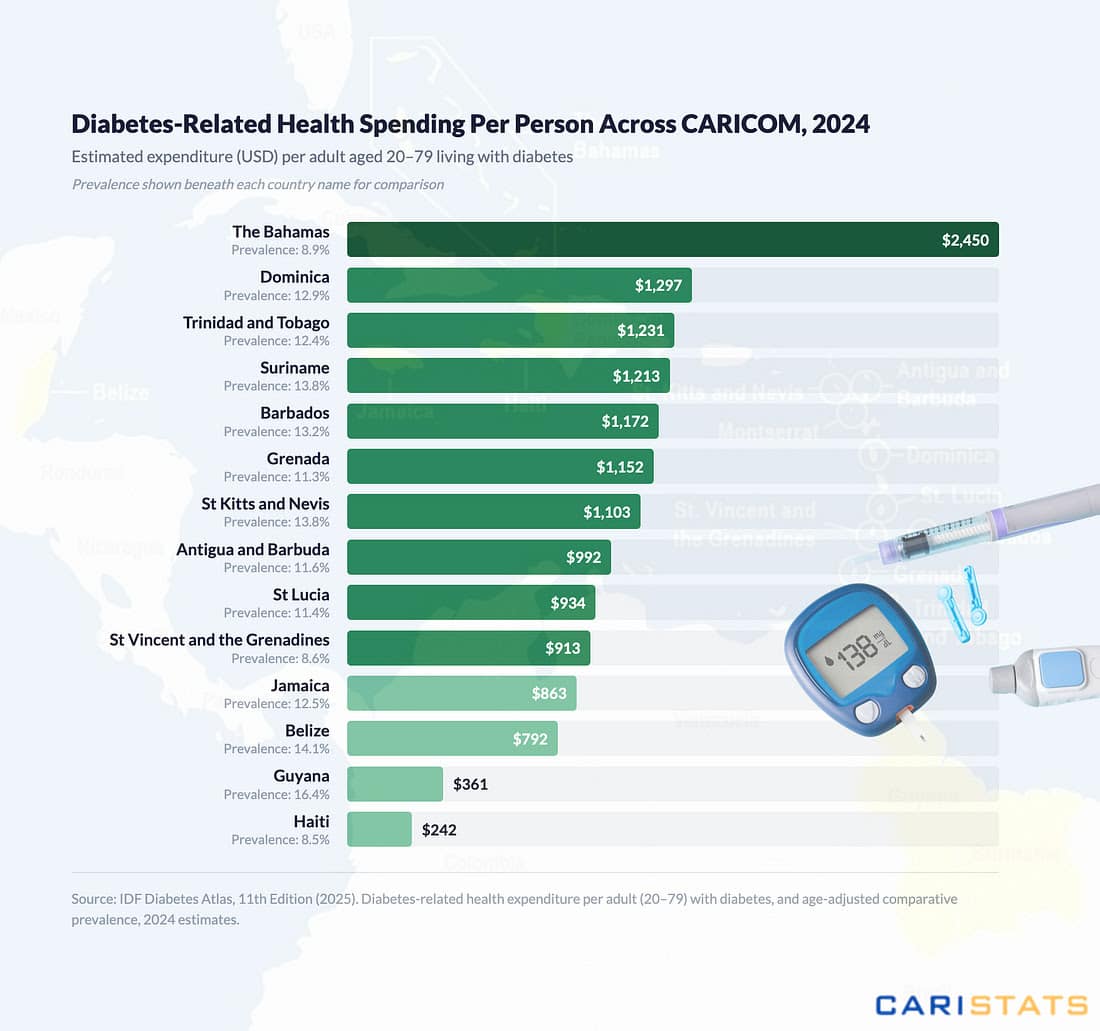
The conference emerges against alarming health statistics: one-quarter of Barbadian adults live with diabetes while hypertension affects 40% of the adult population. Conference Director Fern Lewis emphasized the urgent need for intervention, stating “Longevity is not luck, it’s designed,” highlighting the event’s focus on practical lifestyle modifications including natural movement, plant-based nutrition, and social connectivity.
Featuring 15 international and regional experts including Blue Zones co-founder Nick Buettner, the program will deliver practical longevity strategies through workshops addressing sleep science, nutritional biochemistry, and sexual health. A distinctive feature will be the Blue Wellness Village – an interactive space offering health screenings, personalized consultations, and reimagined Caribbean cuisine demonstrations.
Health officials addressed Barbados’s high disease reporting rates, with Minister Davidson Ishmael explaining: “While it may look like our numbers are high compared to other places, it is because Barbados does a very good job of capturing and presenting information.” He emphasized that proper management can prevent severe complications, urging citizens to “take your medication, exercise, eat properly, and you can live a long, happy life even with the condition.”
The initiative represents DHAB’s 50th anniversary commitment to broadening public engagement. President Tyrone Lowe declared: “We are determined to win this battle not just by medical interventions, but with a shared commitment to healthy living.” Corporate sponsor Republic Bank characterized the health crisis as fundamental to national prosperity, with representative Sharon Zephirin challenging attendees: “When you’re thinking the $300 [conference fee] is too much… ask, ‘What’s your life worth?’”
Chief Medical Officer Dr. Kenneth George emphasized preventive self-care practices and contested international perceptions about Barbados’s amputation rates, asserting efforts to expand podiatric services across the healthcare system.