In a significant move to bolster public health and safety in the aftermath of Hurricane Melissa, ANSA Chemicals Jamaica has pledged a substantial donation of 69,800 litres of bleach. This initiative is designed to support sanitation and water treatment efforts in communities across Jamaica that have been severely affected by the hurricane. The donation comprises two types of bleach: 50,000 litres of eight per cent industrial-strength bleach and 19,800 litres of five per cent household bleach, ensuring that even the most remote areas have access to safe, treated water. Stephen Summers, Country Manager of ANSA Chemicals Jamaica, emphasized the company’s commitment to aiding relief and rebuilding efforts, stating, ‘This donation is part of our ongoing commitment to the people of Jamaica in their time of need.’ The distribution will be managed by the Office of Disaster Preparedness and Emergency Management (ODPEM), with plans to deliver three to five industrial totes and one container of household bleach daily. Matthew Samuda, Minister of Water, Environment and Climate Change, praised the partnership, highlighting the critical role of sanitation in preventing public health crises post-disaster. Commander Alvin Gayle, Director General of ODPEM, also welcomed the donation, noting its importance in maintaining public health and safety. ANSA Chemicals Jamaica, a leading provider of chemical products in the Caribbean, continues to play a vital role in enhancing community well-being through such initiatives.
分类: health
-
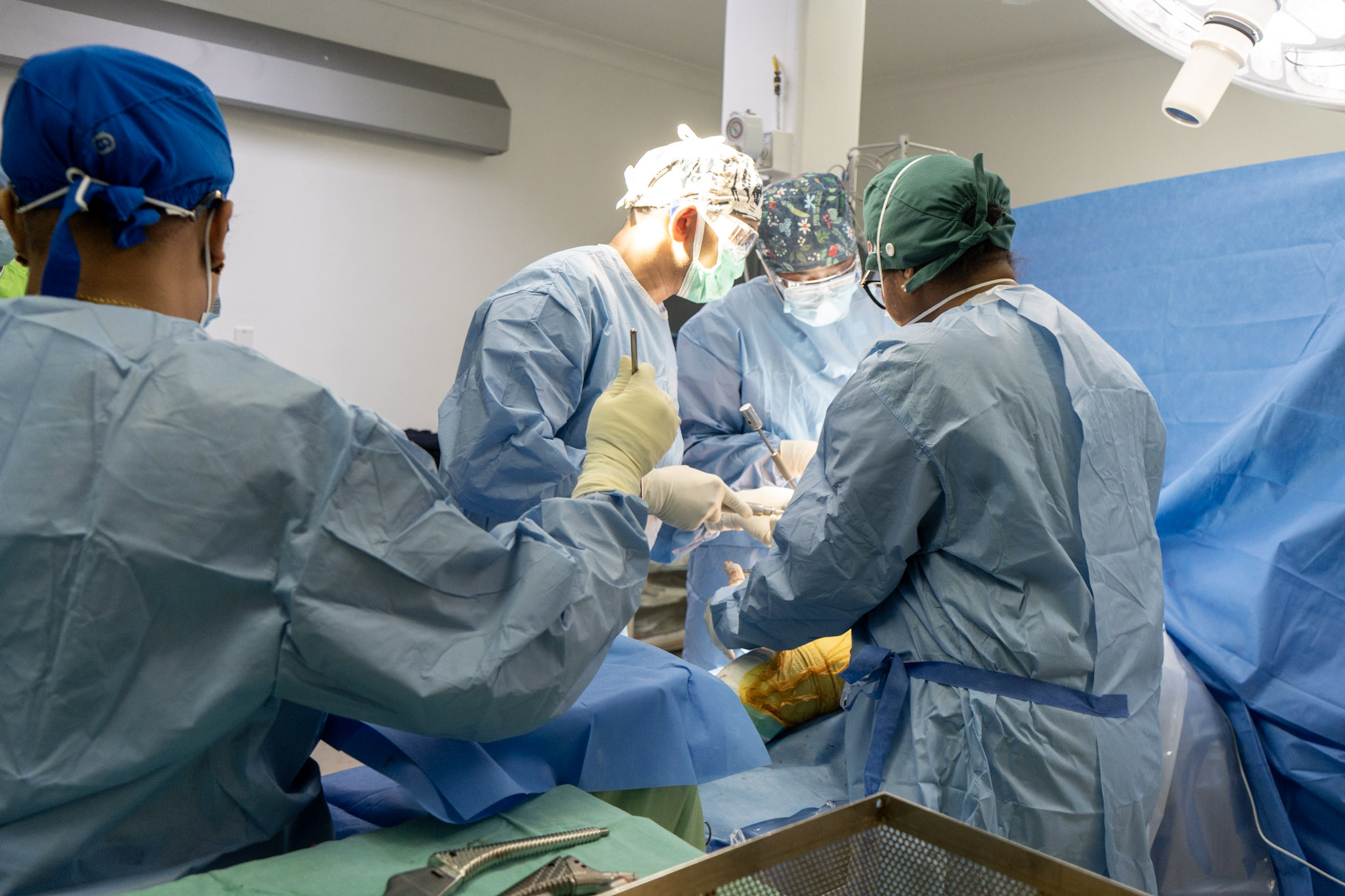
GPHC successfully completes 28 joint replacement surgeries
The Orthopaedic Department at Georgetown Public Hospital Corporation (GPHC) has marked a significant achievement by successfully completing 28 joint replacement surgeries during a concentrated three-day initiative. This remarkable feat, which took place from November 7th to 10th, 2025, underscores the department’s growing expertise and efficiency in delivering high-quality orthopaedic care. The surgeries, comprising 18 knee replacements and 10 hip replacements, provided life-changing relief to 22 female and 6 male patients, all of whom have since been discharged. Led by Dr. Kaaleshwar Ramcharran, the dedicated team of orthopaedic surgeons, anesthetists, physiotherapists, nurses, and operating theatre staff surpassed their initial target of 27 procedures, demonstrating exceptional teamwork and commitment. Joint replacement surgeries are among the most transformative medical interventions, offering renewed mobility and quality of life to individuals suffering from severe joint pain or disability. In private institutions, such procedures can cost approximately GY$2.5 million per surgery, highlighting the immense value of GPHC’s initiative to its beneficiaries. The hospital’s management praised the orthopaedic team for their unwavering dedication and compassionate care, emphasizing their role in advancing surgical services, improving patient outcomes, and reducing waiting times for essential procedures. This achievement reflects GPHC’s ongoing investment in enhancing healthcare infrastructure and delivering world-class medical services to the people of Guyana.
-

Tackling this epidemic as we did with COVID-19
In response to a surge in nonspecific febrile syndrome cases primarily caused by arbovirus infections, Cuban President Miguel Díaz-Canel has announced weekly meetings to analyze the situation and propose solutions. The decision follows a gathering of health experts and scientists at the Palace of the Revolution, where the President emphasized the need for a coordinated approach akin to the nation’s COVID-19 response. The meeting, attended by Deputy Prime Minister Eduardo Martínez Díaz and prominent health specialists, focused on the current epidemiological landscape, particularly the spread of dengue, Chikungunya, and Oropouche viruses. Dr. José Raúl de Armas Fernández reported a decline in febrile cases across eight provinces but highlighted the persistence of arbovirus transmission in 38 municipalities, with Havana being notably affected. Chikungunya cases have surged to 21,681, concentrated in six provinces, while Oropouche cases remain absent since September. Dr. María Guadalupe Guzmán Tirado underscored the global prevalence of Chikungunya and Cuba’s intensified surveillance efforts. Dr. Yagen Pomares Pérez, Director General of Primary Health Care, stressed the importance of early fever detection and patient isolation, drawing parallels to lessons learned during the pandemic. She emphasized the need for hospitalizing vulnerable groups, including children under two, pregnant women, and older adults with comorbidities. Dr. Madelaine Rivera Sánchez, National Director of Surveillance and Vector Control, highlighted challenges in fumigation efforts and called for community participation to enhance vector control measures. The government aims to address equipment shortages and logistical issues to curb the epidemic’s spread effectively.
-

Americas lose Measles-Free Status as Canada records sustained cases
The Pan American Health Organization (PAHO) has raised alarms over the resurgence of measles in the Americas, as Canada reports sustained transmission of the disease for over 12 months. This development has led to the region losing its measles-free status, a significant setback in public health efforts. Measles, known for its high contagion rate, is particularly concerning with the winter travel season approaching, increasing the risk of widespread transmission across the Americas. Dr. Sealy, PAHO’s Assistant Director, emphasized the importance of achieving a 95% vaccination coverage for both doses of the MMR (measles, mumps, and rubella) vaccine, noting that while the Caribbean maintains strong vaccination rates, there has been a decline in second-dose administration in some areas. PAHO officials are urging countries to bolster vaccination efforts and encourage individuals to report symptoms promptly to prevent further spread. Dr. Jarbas Barbosa, PAHO’s Director, acknowledged the setback but stressed that the situation is reversible, highlighting the ongoing global threat of measles outbreaks. Health authorities remain vigilant as active cases persist in the United States, Mexico, and Venezuela.
-

PAHO – alert: America’s verliezen status mazelenvrije regio
The Pan-American Health Organization (PAHO) has announced that the Americas region has lost its status as free from endemic measles transmission. This decision follows the findings of PAHO’s Regional Commission for Monitoring and Re-verification of Measles, Rubella, and Congenital Rubella Syndrome Elimination, which convened in Mexico City from November 4 to 7, 2025, to assess the epidemiological situation in the region. The commission confirmed that endemic measles transmission has re-emerged in Canada, where the virus has been circulating for at least twelve months. This marks a significant setback for the Americas, which was the first region globally to eliminate measles twice. All other countries in the region retain their elimination status for now. PAHO Director Dr. Jarbas Barbosa emphasized that while this loss is a setback, it is reversible. He stressed that as long as measles persists globally, the region remains at risk of reintroduction and spread among unvaccinated or under-vaccinated populations. With political will, regional cooperation, and sustained vaccination efforts, transmission can be interrupted, and the shared success of elimination restored. As of November 7, 2025, 12,593 confirmed measles cases have been reported across ten countries, with 95% of cases concentrated in Canada, Mexico, and the United States. This represents a thirtyfold increase compared to 2024. Tragically, 28 deaths have been recorded, with 23 in Mexico, 3 in the U.S., and 2 in Canada. Active outbreaks are ongoing in Canada, Mexico, the U.S., Bolivia, Brazil, Paraguay, and Belize, primarily driven by imported cases. Most infections occur in under-vaccinated communities, with 89% of cases involving unvaccinated or vaccination-status-unknown individuals. Children under one year old are the most affected, followed by those aged one to four. The Canadian outbreak began in October 2024 in New Brunswick and spread nationwide, with over 5,000 confirmed cases. While new cases are declining, transmission persists in Alberta, British Columbia, Manitoba, and Saskatchewan. Measles, one of the most contagious viruses, can infect up to 18 people per case and lead to severe complications such as pneumonia, encephalitis, blindness, and death. Outbreaks also strain healthcare systems. Vaccination remains the most effective tool against measles, having prevented an estimated six million deaths in the Americas over the past 25 years and 15 million globally in the last 50 years. However, the regional coverage rate for the second dose of the MMR vaccine was only 79% in 2024, well below the 95% threshold needed to prevent outbreaks. PAHO continues to support countries in strengthening surveillance, laboratory diagnostics, outbreak response, and vaccination campaigns. Experts have been deployed to Mexico, Argentina, and Bolivia, while the organization closely monitors Belize, Brazil, and Paraguay. Dr. Barbosa urged countries to redouble their efforts, emphasizing that every prevented outbreak and stopped infection saves lives. The commission recommended intensifying vaccination campaigns, enhancing electronic immunization registries, sustainably funding laboratory capacity, and conducting PCR tests for suspected cases with negative IgM results. The Americas have previously regained measles-free status after temporary losses in Venezuela (2018) and Brazil (2019) through coordinated regional action. To regain the status, a country must demonstrate no endemic transmission for at least twelve consecutive months, supported by vaccination, surveillance, and outbreak response data. Canada is now implementing an action plan within PAHO’s regional framework to increase vaccination rates, strengthen monitoring systems, and respond swiftly to new outbreaks. Dr. Barbosa concluded, ‘Collaboration, solidarity, and science are stronger than any virus. When we work together, we protect the health and lives of all people in the Americas.’
-

Uruguayan government prioritizes mental health care
Cristina Lustemberg, Uruguay’s Minister of Public Health, has raised alarms over the escalating mental health crisis in the country, revealing that 30,000 individuals are currently awaiting treatment for mental health conditions. Speaking at the launch of the “National Action for Mental Health” initiative, Lustemberg emphasized the need for an interdisciplinary approach to address the issue. She criticized the uneven access to mental health care, stating, “It cannot be that, despite having an Integrated National Health System, access to mental health care remains a privilege in some areas.”
The initiative, developed through the collaboration of over 20 working groups, aims to tackle mental health challenges by prioritizing community-driven issues, fostering regional and inter-institutional networks, and integrating cultural, sports, and educational spaces. Funding has been allocated to support these efforts, including strengthening agreements with the State Health Services Administration, the Ministry of Social Development, and departmental governments. Additionally, resources will be directed toward suicide prevention programs.
A key component of the plan is the appointment of a mental health coordinator in each of the country’s departments to oversee the implementation of the initiative. This move comes as Uruguay faces a significant mental health burden, with 29% of the adult population exhibiting symptoms of psychological distress and 24% experiencing severe loneliness. The initiative represents a critical step toward addressing these pressing issues and ensuring equitable access to mental health care nationwide.
-

More health centres opened in St Elizabeth post Melissa
In a significant move to enhance healthcare accessibility, the Southern Regional Health Authority (SRHA) has announced the reopening of multiple health centers across St Elizabeth, Jamaica. These facilities are now operational to provide essential primary care services to residents in the parish. The reopened centers include Junction, Portsea, Malvern, Santa Cruz, Pepper, Myersville, Lacovia, Balaclava, Maggotty (Holy Spirit Church), Elderslie (mobile unit), Southfield, Bellevue, Newell, Black River (tent), New Market (mobile unit), Gingerhill (medical outreach), and Middle Quarters. Operating hours are set from Monday to Thursday, 8:30 am to 4:30 pm, and on Fridays from 8:30 am to 4:00 pm. The SRHA has clarified that specific services will be available on designated days, ensuring a structured approach to healthcare delivery. This initiative aims to address the growing healthcare needs of the community, particularly in underserved areas, and marks a pivotal step in improving public health infrastructure in the region.
-

Unsafe to eat
In the wake of Hurricane Melissa, which struck Jamaica on October 28, the Public Health Department has ordered the destruction of 5,661 kilogrammes of food deemed unsafe for consumption. The decision followed inspections of 5,052 food handling establishments, as disclosed by Minister of Health and Wellness Dr. Christopher Tufton in Parliament on Tuesday. The hurricane, a Category 5 storm, left several south-western parishes without electricity, severely disrupting food safety and public health systems.
Dr. Tufton emphasized the government’s efforts to monitor large farms and food processing facilities to prevent unsafe food from entering the supply chain and to avert potential outbreaks of food-borne diseases. He assured that safety measures would be intensified as access to previously marooned communities improves. Opposition health spokesman Dr. Alfred Dawes echoed the need for vigilance, warning that diseases such as dysentery, dengue, and cholera could emerge in the aftermath of the disaster.
The hurricane caused catastrophic damage to health infrastructure across the island, particularly in the southern and western regions. Seven hospitals, including Black River, Noel Holmes, and Cornwall Regional, suffered extensive roof and structural damage. A field hospital has been established in Black River, with plans for additional facilities in Falmouth and Savanna-la-Mar. Over 100 health centres also reported damage, severely impacting primary care services.
Despite these challenges, the Ministry of Health has initiated a three-phase recovery plan. The first phase focuses on restoring basic health services, preventing disease outbreaks, and addressing staff welfare. Dr. Tufton highlighted that 79% of healthcare professionals have returned to work, enabling the resumption of critical services such as maternal and child health care, HIV treatment, and immunizations in 30% of damaged facilities.
The government’s response also includes mass environmental health actions, psychosocial interventions, and infrastructure repairs. Dr. Tufton stressed the importance of rebuilding the health system to be more resilient, stating, ‘We must build back better.’ The Ministry continues to urge citizens to practice proper hygiene, use safe water sources, and report any illness symptoms promptly.
-

Bodoe: Include wellness in HSE framework
In a compelling address at the American Chamber of Commerce’s TT (Amcham TT) 15th Annual National Excellence in HSE Awards ceremony, Trinidad and Tobago’s Health Minister, Dr. Lackram Bodoe, emphasized the urgent need to evolve the traditional Health, Safety, and Environment (HSE) framework into a more comprehensive model that includes wellness. The event, held on November 10 at the Hyatt Regency in Port of Spain, brought together key stakeholders to discuss the critical role of HSE in safeguarding both human lives and economic productivity.

